ADHD: A trending diagnosis at what cost
August 1, 2023
A trend or a diagnosis
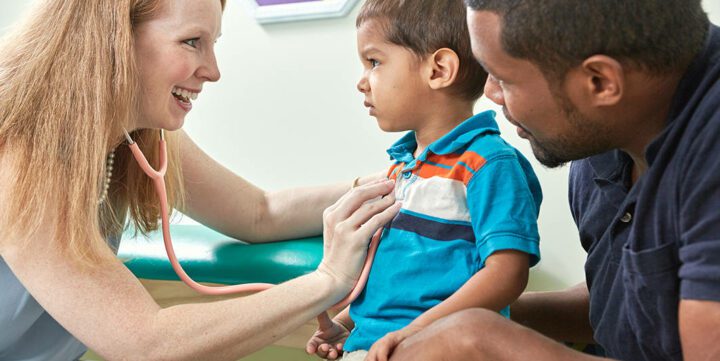
Attention Deficit Hyperactivity Disorder (ADHD) is a neurodevelopmental disorder that is increasingly recognized not only in childhood but also in adulthood. Characterised by difficulties with attention, hyperactivity, and impulsiveness, ADHD has a significant impact on a person’s daily functioning and quality of life. Despite being a common condition, ADHD is surrounded by myths, misconceptions, and an often overlooked societal issue – healthcare access.
In recent years, Australia has seen a surge in ADHD diagnoses. Alongside this rise, a significant challenge has emerged: the lack of accessible and affordable healthcare services for people with ADHD or seeking diagnosis. As it stands, only psychiatrists and paediatricians can confirm a diagnosis of ADHD and prescribe certain medications associated. This exclusive system creates a significant barrier for many seeking help, particularly when faced with the exorbitant costs associated with private psychiatric services.
Meanwhile, the public health system struggles under the weight of significant mental health demand, leaving many patients underserved or even untreated throughout the wake of the pandemic. This growing issue is further complicated by ongoing debates within the medical community regarding the diagnostic nature of ADHD and the most effective treatment strategies. Among these growing concerns lies a further debate into the over-diagnosis of conditions such as ADHD, and what this means for communities at large.
Rising needs receiving slow response
Current media discussions have shed light on the increasing demand for ADHD diagnosis and treatment, and the associated expenses that have become a cause for concern. A recent trend on TikTok, where users post content related to their ADHD experiences, has garnered over 20 billion views. Creators argue these videos spread awareness and normalise the condition, yet they may inadvertently contribute to a heightened demand for diagnostic services.
In Australia, this surge has exposed a critical issue: the prohibitive cost of seeing a psychiatrist for ADHD diagnosis and treatment. Presently, only psychiatrists and paediatricians can confirm ADHD diagnoses and provide access to the necessary medication, restricting GPs’ involvement in this area. The medication, largely unchanged over the years, primarily influences the central nervous system’s dopamine system, paradoxically slowing the fast-paced thoughts of an ADHD individual rather than inducing hyperactivity. The nature of ADHD as a disorder requiring treatment or as a normal variant needing medication remains a contentious issue, with invested stakeholders on both sides.
According to a 2019 report by Deloitte on the Social Costs of ADHD in Australia, ADHD affects approximately 281,200 children and adolescents (aged 0-19) and 533,300 adults (aged 20+) in Australia. Despite numerous initiatives and increasing awareness, the reality remains: our society harbours a two-tier system for mental health care. Both the public and private systems, funded by Medicare and health insurance premiums respectively, are under-resourced and underserved. The lucrative engagement of psychiatrists in private ADHD clinics creates a disturbing third tier, indicative of a troubling trend that could further exploit consumer demand and disengage professionals from existing health systems.
The role of general practitioners in addressing ADHD
Dr. Nicole Higgins, president of the RACGP, highlights a substantial gap in the ADHD healthcare landscape. She notes the hardship faced by many patients in securing care for their condition, signifying a clear call to action for GPs to expand their role in diagnosing and managing ADHD. “Access to ADHD diagnosis is inadequate and unaffordable for too many patients,” she said.
The evidence points to a growing demand for ADHD diagnosis. As per an RACGP poll from March 2023, nearly 78% of respondents reported a substantial increase in patient inquiries about referrals for ADHD diagnosis in the last 12 months, with another 16% reporting a modest increase.
Unfortunately, the ability of GPs to fully engage in the diagnosis and management of ADHD is currently impeded by jurisdictional disparities in rules surrounding ADHD diagnosis and prescription of stimulant medications. For instance, while GPs in Queensland and New South Wales can diagnose ADHD and prescribe stimulant medication under certain circumstances, this is not a nationwide practice.
However, the future could be different. Initiatives where GPs collaborate with paediatricians and psychiatrists to enhance their skills in diagnosing and managing ADHD are currently in progress or proposed in several regions, including Western Australia, Queensland, New South Wales, and Victoria. This situation has led to what Dr. Higgins describes as a “postcode lottery,” indicating a dire need for uniformity across all states and territories. The goal should be consistent rules detailing which clinicians are authorised to diagnose ADHD and prescribe stimulant medications, and these should unequivocally include GPs. “Some GPs have already taken on an increased role in diagnosing and treating ADHD, but more support and regulatory change is needed,” Dr Higgins said.
To facilitate this, local, state, and Commonwealth governments should coordinate funding for models of care that support shared care approaches and clear health pathways for patients. Patients’ access to care would also improve with higher rebates for relevant Medicare-subsidised services.
Moreover, Dr. Higgins emphasises the importance of providing lifelong, individualised support for those living with ADHD, often alongside other conditions like autism spectrum disorder, depression, anxiety, and sleep disorders. As such, a comprehensive, regularly reviewed care plan led by a patient’s usual GP and backed by a multidisciplinary team is critical. Ensuring affordable access to allied health services, such as psychology, is also essential for improving patient care.
Systemic change is imminent
Late last year, the Parliament of Australia looked to public and private input with an inquiry into “Barriers to consistent, timely and best practice assessment of attention deficit hyperactivity disorder (ADHD) and support services for people with ADHD” where they have sought the opinions of GPs and varying physicians as to who is best equipped to take on this rapid rise in diagnosis.
There’s a pressing need to address the gaps in healthcare for ADHD patients, a responsibility that falls onto the broader medical community, particularly education providers. As demand for ADHD diagnosis and treatment escalates, the health system is grappling with the strain, further underscoring the urgency to arm GPs with the appropriate skills and knowledge to diagnose and manage this prevalent condition.
The future of ADHD diagnostics
Historically, ADHD diagnosis and treatment have predominantly been the province of psychiatrists and paediatricians, leaving GPs relatively sidelined. However, the tides are changing, with an increasing call for GPs to play a more robust role in this space. Education providers have a crucial responsibility here: to equip GPs with in-depth knowledge of ADHD, its diagnostic process, and effective management strategies.
The benefits of a well-informed and capable GP in diagnosing and managing ADHD extend beyond the individual patient. A GP, with their long-term, holistic knowledge of a patient’s health, is often best positioned to recognize, diagnose, and manage ADHD, leading to faster and more efficient care. This streamlined care pathway would not only alleviate the burden on patients, but also greatly reduce the stress on our overwhelmed health system.
Education providers need to act now, developing comprehensive training programs that incorporate the latest research and clinical guidelines on ADHD. These programs should aim to provide GPs with a thorough understanding of ADHD, from recognizing its symptoms and managing comorbid conditions, to navigating the complex landscape of ADHD medications.
Further, these training programs must also focus on equipping GPs with the skills to support their ADHD patients beyond the clinical aspect, helping them understand and manage the impact of ADHD on their daily lives. This holistic approach will allow GPs to offer their patients comprehensive care, thereby improving patient outcomes and satisfaction.
By investing in the education of GPs, we can mitigate the pressure on specialists and reduce wait times for patients, fostering a more accessible and equitable healthcare system. Consequently, education providers have a critical role to play in this initiative. Their commitment to enhancing GPs’ understanding and skills in diagnosing and managing ADHD can pave the way for a much-needed revolution in ADHD healthcare.